In breathless language, the human rights organization Amnesty International urges the US to confront its “shocking maternal mortality rate.” Entitled Deadly Delivery: The Maternal Healthcare Crisis in the USA, the Amnesty report lays its indictment:
The total amount spent on health care in the USA is greater than in any other country in the world. Hospitalization related to pregnancy and childbirth costs some US$86 billion a year; the highest hospitalization costs of any area of medicine. Despite this, women in the USA have a greater lifetime risk of dying of pregnancy-related complications than women in 40 other countries… More than two women die every day in the USA from pregnancy-related causes…
Amnesty International is sure that this increase in maternal mortality is due to lack of access to medical care.
The US government’s failure to ensure that women have guaranteed lifelong access to quality health care, including reproductive health services, has a significant impact on the likelihood of having a healthy pregnancy and delivery.
“Natural” childbirth advocates are sure that the rising rate of C-sections and other interventions is contributing to the rising maternal mortality rate. Amnesty International appears to agree, citing a “lack of information and autonomy” as the cause.
Both decreased access and increased interventions are plausible causes of increased maternal mortality. However, it is far from clear that maternal mortality is even rising, let alone that it is rising because of decreased access to care or increases in the C-section rate or other interventions. A careful review of the data suggests that changes in the way that maternal mortality is assessed may be leading to a spurious “increase” in maternal mortality. Moreover, a detailed analysis of the causes of maternal mortality casts serious doubt on either access or interventions as the cause of any rise.
In the last two decades, there has been growing awareness that maternal mortality is under-reported. Vigorous efforts have been made to correct that problem, by both increasing surveillance and expanding categories included within maternal mortality. The CDC report Maternal Mortality and Related Concepts (2007) explains these changes:
In 1999, the coding guidelines used in the United States were expanded to cover additional categories … Furthermore, if only indirect maternal causes of death (i.e., a previously existing disease or a disease that developed during pregnancy that was not due to direct obstetric causes but was aggravated by physiologic effects of pregnancy) were reported in Part I and pregnancy was reported in either Part I or II, the death was classified as a maternal death. [Previously] the pregnancy had to be reported in Part I for the death from indirect causes to be considered a maternal death.
Along with the new definitions, the [new coding guidelines] introduced new details and categories in the cause-of-death titles associated with pregnancy, childbirth, and the puerperium…
Furthermore, in 2003, the US Standard Certificate of Death was revised to ask explicitly whether any female death was associated with pregnancy, instead of relying on the person filling out the form to voluntarily provide that information.
The results of these changes are captured by the following graph.

It is clear that the 1999 and 2003 changes in reporting of maternal mortality resulted in large “increases” that are not increases at all. They reflect the more accurate measurement of maternal mortality just as they were designed to do.
Yet some of the increase may be real. What about possible causes?
Curiously, since Amnesty International bases its entire report on the claim that decreased access to healthcare has led to increased maternal mortality, the report contains no evidence that there has been a decrease in access to maternity services. While millions of people lack health insurance, almost all states provide public health insurance for the duration of pregnancy in any woman who needs it. Indeed, 99+% of births take place in hospitals, so there is certainly no decrease in access to hospital care.
If decreased access to healthcare were responsible for an increase in maternal mortality, we would expect that the increase would be spread evenly among all possible causes of maternal mortality, but that’s not what we find. The following chart shows maternal death rates from pre-eclampsia/eclampsia, hemorrhage, embolism (the three most common causes of maternal death) as well as other direct causes (all other obstetric complications) and indirect causes (from other medical conditions).
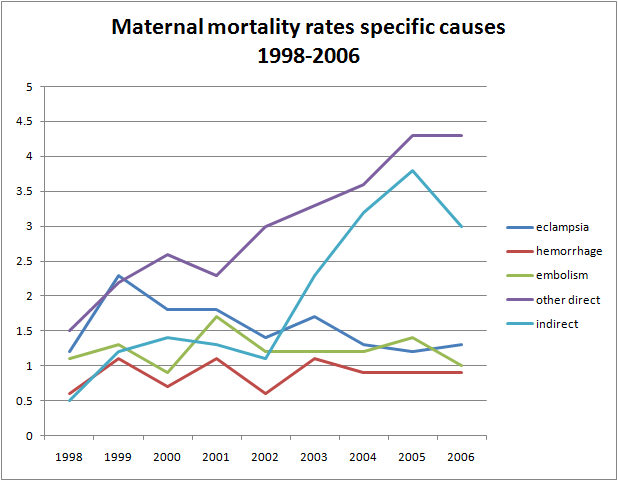
As the graph shows, the purported increase in maternal mortality was not spread evenly across all categories. Indeed, the most common cause of maternal mortality remained flat. In contrast, the categories that were expanded in the new reporting guidelines were responsible for almost all of the purported increase. This suggests that the “increase” reflects more comprehensive reporting, not an actual increase in maternal mortality.
What about an association between the rising C-section rate and rising maternal mortality? A graph comparing the maternal mortality rate and the C-section rate certainly shows a correlation.

But correlation is not causation. If the rising C-section rate were leading to an increased maternal mortality rate, we would expect to see C-section complications, such as hemorrhage and embolism increasing disproportionately. But that’s not what we see. As the following graph makes clear, both hemorrhage and embolism death rates did not change their contributions to overall maternal mortality.
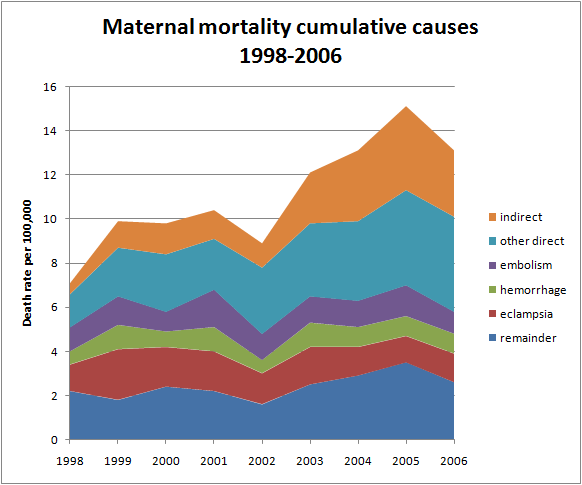
The fact that hemorrhage and embolism were flat casts doubt on the idea that the increasing C-section rate is leading to increasing maternal mortality. Moreover, the C-section rate rose from 2005 to 2006, but the maternal mortality rate actually dropped.
So what can we conclude about the observed rise in maternal mortality? First, we can see that the 1999 coding revision and the 2003 birth certificate revision captured more maternal deaths just as they were designed to do. Those increases almost certainly reflecting changes in reporting and not increases in maternal mortality. Together they account for 80% of the observed increase since 1998 (5/100,000 out of a total change of 6.2/100,000). With that in mind, the Amnesty International report can be described as overwrought, to say the least.
And to the extent that there has been a real increase, is decreased access or the increased C-section rate the causes of this increase? That seems unlikely since the increase was not distributed evenly among all causes (as would be expected if decreased access were to blame) nor is the increase predominantly distributed among common C-section complications (if the increased C-section rate were to blame).
Despite the rhetoric of Amnesty International, it is unclear whether we are experiencing a crisis of any kind, let alone a “shocking” maternal mortality rate.













