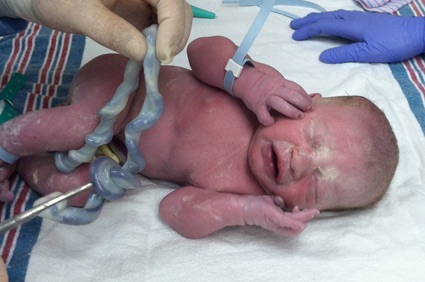
Natural childbirth and homebirth advocates get very excited about umbilical cords, specifically nuchal (neck) cords, the medical term for an umbilical cord that gets wrapped around the baby’s neck. They get excited because they believe that obstetricians dramatize the risk of nuchal cords (“the baby could die”) when they aren’t dangerous at all. As usual, natural childbirth and homebirth advocates are wrong on this point and the reason is that they fundamentally misunderstand when and why a nuchal cord dangerous.
How does an umbilical cord get wrapped around the baby’s neck in the first place. The reason is that for most of pregnancy, the baby has a lot of room to move and the cord is relatively long. Moving around, up and down, and somersaulting, the baby can easily get the cord wrapped around itself. Most of these loops will slip off at some point, generally without causing a problem. There is the possibility, however, that even if the loops eventually slip off the baby, a true knot will have been formed but many true knots never cause a problem.
[pullquote align=”right” color=”#5A70C6″]To understand the danger of a nuchal cord it helps to think of the cord as similar to the air line of a deep sea diver. [/pullquote]
Even more likely, a loop may get stuck around the neck because it is more slender than the shoulders below it and the head above it. Contrary to popular belief, the danger of a nuchal cord has nothing to do with the fact that it is wrapped around the baby’s neck. Since the fetus does not breathe, compressing its neck has no impact on whether there is adequate oxygen in the blood. In other words, the effect of neck compression is fundamentally different than if the neck of a child or adult is compressed.
In order to understand the danger of a true knot in the cord or a nuchal cord it helps to think of the cord as similar to the air line of a deep sea diver. It’s easy to understand that if a diver moved around such that he created a true knot in an air line, it could pose a serious problem. If the knot isn’t pulled tight, there is no problem. The oxygen can pass easily through the loop. However if the knot gets pulled tight because the diver pulls on the air line by diving down deep or it gets pulled tight by being snagged on something else, the supply of oxygen can get cut off and the diver could die.
Similarly, a loose true knot in the umbilical cord is not a problem for the fetus because the oxygen continues flowing through the loop. However, if the knot gets pulled tight, either by the cord being pulled as the baby descends into the pelvis or the cord getting pulled by being snagged on an arm or leg, the baby will be deprived of oxygen and die
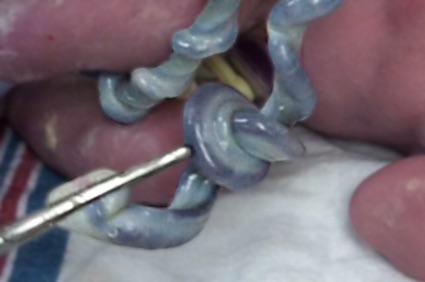
This picture of a true knot (a close up of the picture at the top) was sent to me by a reader. It was noted at her 3rd C-section. It is easy to understand that had the knot been pulled tighter, the baby might have died..
If an air line got wrapped loosely around a diver’s neck, the oxygen would keep flowing through it. However if the loop or loops were so tight as to cut off flow within the line, the diver will die. Of course a diver could actually be strangled by a loop or loops of cord, but a baby cannot. Therefore, the issue with a nuchal cord is NOT the fact that it is wrapped around the neck. The issue is whether the loop is pulled tight enough to cut off the flow of blood and therefore of oxygen.
The bottom line is that true knots of cord are not necessarily dangerous, but there is no way to no beforehand whether the knot will tighten during the course of labor and cut off oxygen to the baby. Similarly, a nuchal cord is not necessarily dangerous; in fact most nuchal cords are loose and therefore do not threaten the baby. Once again, though, there is no way to know beforehand how the loop or loops around the neck will be affected during labor. The higher the number of loops, the shorter the remaining cord, and the more likely that the cord will be fatally compressed during labor. However, even a single loop can be pulled tight during the descent of the baby and the baby will die for lack of oxygen.
Ultimately, when NCB and homebirth advocates “trust birth,” they are trusting that there are either no knots or loops in the cord, or that if they exist, they will not be pulled tight. But that makes no more sense than a deep sea diver trusting that he can assume that there are no knots in his air line and not worry if the air line gets wrapped around his neck. Obviously, in the case of the air line, trust has nothing to do with it, and, in direct contrast to what NCB and homebirth advocates proclaim, in the case of the umbilical cord, trust has nothing to do with the presence or absence of knots and loops.
The only way to know if a knot or nuchal cord is hindering the flow of the blood to the baby is to monitor the baby’s heart rate. Without monitoring, the supply of oxygen to the baby could completely stop during labor and no one would know until the baby was born dead.
This piece first appeared in February 2012.