
As a society, we invest in public health campaigns because they provide two main benefits: improved health of populations and cost savings.
But what if a public health campaign provided neither?
It’s World Breastfeeding Week 2019 and it’s time to ask: where is the return on investment in breastfeeding promotion?
[perfectpullquote align=”right” cite=”” link=”” color=”” class=”” size=””]It’s time to end the fiction that breastfeeding has a public health benefit.[/perfectpullquote]
For 25 years, we’ve been told that it was worth spending millions on breastfeeding campaigns because the result would be improved health for infants, children and adults. Where are the improvements? For 25 years, we’ve been told to spend ever more because we would glean massive healthcare savings. Where are the savings?
What does it look like when a public health campaign leads to improved health?
Vaccination has provided spectacular gains. There have been dramatic reductions in both cases of disease and deaths from disease.
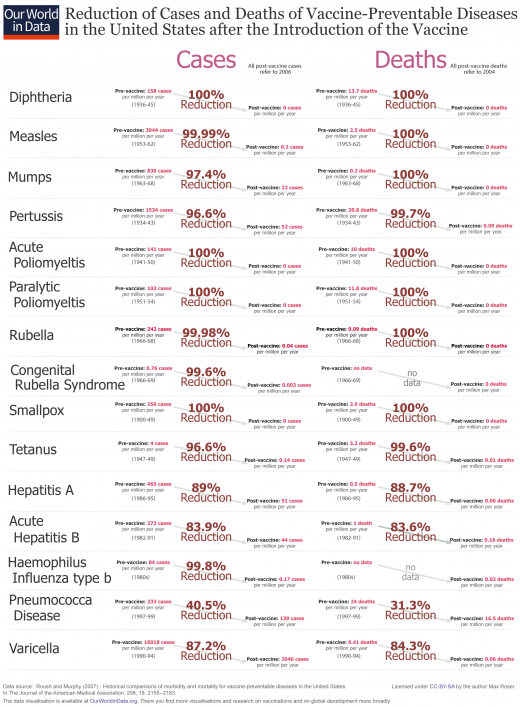
Vaccination didn’t merely reduce the incidence of vaccine preventable diseases, it often resulted in NO CASES at all. Vaccination didn’t merely reduce the number of deaths from vaccine preventable diseases, in some cases it ELIMINATED them entirely.
It is important to note that these are not theoretical benefits. This is what actually happened when vaccination programs were implemented.
Let’s look at another public health campaign, the effort to reduce lung cancer from tobacco smoking. The results have not been as spectacular, but are impressive nonetheless.

In the wake of the Surgeon General’s 1964 report warning about the link between smoking and lung cancer, per capita cigarette consumption dropped dramatically. After a lag period, lung cancer deaths began to drop dramatically, too. This is not a theoretical benefit. This is what actually happened.
In the past 25 years we have spent millions of dollars promoting breastfeeding even though the scientific evidence on the benefits is weak, conflicting and riddled with confounding variables.
An entire industry, the breastfeeding industry, has arisen to promote and profit from efforts to increase breastfeeding rates. Lactation consultants did not exist prior to the mid 1980’s. Now they are everywhere, in hospitals, in doctors’ offices and in independent practice.
A private company, Baby Friendly USA, is allowed into hospitals to promote their philosophy. For a fee of more than $10,000, a hospital can to be designated as breastfeeding friendly — but only if it is in lockstep with the practices recommended by the breastfeeding industry.
Breastfeeding initiation rates have risen in response. But the breastfeeding rate appears to have had no impact on the infant mortality rate. The graph below illustrates the steep drop in infant mortality over the course of the 20th Century. I’ve added markers for the breastfeeding rate at various points. As you can see, the precipitous drop in breastfeeding rates did not have an impact on infant mortality and the rising rate of breastfeeding initiation does not seem to have an impact, either.

The only measurable impact has been the reduced incidence of necrotizing enterocolitis among very premature infants, a benefit that was not predicted but was found as breastfeeding rates rose.
There are papers predicting health and spending benefits of breastfeeding, but I haven’t found any evidence of actual benefits, with one exception: the reduced incidence of necrotizing enterocolitis among very premature infants, a benefit that was not predicted but was found as breastfeeding rates rose. If other benefits actually occur, I invite anyone who has seen the evidence to share it with the rest of us. Otherwise, we must conclude that — unlike vaccination efforts and efforts to reduce smoking — the benefits are purely theoretical and therefore probably not real.
Moreover, there is a growing body of evidence that the aggressive promotion of breastfeeding is harming babies through dehydration and starvation due to insufficient breastmilk (affecting up to 15% of first time mothers). Exclusive breastfeeding is now the LEADING risk factor for newborn hospital readmission. It is nothing short of appalling that 1 in 71 breastfeeding newborns will be readmitted to the hospital. That’s tens of thousands of hospitalizations per year at a cost of hundreds of millions of dollars.
That doesn’t mean that breastfeeding is a bad thing. It’s a good thing, but the benefits for term babies in first world countries are trivial. If those benefits were anything other than trivial, we should have seen a dramatic impact on infant health and pediatric care expenditure by now, but we haven’t seen anything of the kind.
No doubt the lactation industry has benefited. The number of lactation consultants in the US has increased from 0 in 1980 to approximately 14,000 lactation consultants in 2013.
What do the rest of us have to show for it?
Nothing.
Unless, of course, you count the soul searing guilt and feelings of inadequacy among women who can’t or choose not to breastfeed.
It’s World Breastfeeding Week 2019 and it’s time to admit that breastfeeding promotion has been an expensive failure.
Going forward we should dramatically scale back spending on breastfeeding promotion. In an era of scarce healthcare dollars, we can’t afford to waste millions on public health campaigns that produce no discernible return on investment.
It’s time to end the fiction that breastfeeding has a public health benefit. It’s a personal choice, no more, no less. There is no reason — scientific or economic — to spend millions promoting it.