
According to The Guardian:
Sweden has cancelled a major study of women whose pregnancy continued beyond 40 weeks after six babies died.
The research was halted a year ago after five stillbirths and one early death in the babies of women allowed to continue their pregnancies into week 43.
“Our belief is that it would not have been ethically correct to proceed” with the study, the researchers concluded.
Not only would it have been unethical to proceed, it was unethical to undertake the study in the first place. The death of babies was not merely preventable; it was inevitable.
[perfectpullquote align=”right” bordertop=”false” cite=”” link=”” color=”” class=”” size=””]Swedish researchers withheld the known preventive treatment for postdates pregnancy deaths to see what would happen.[/perfectpullquote]
Why is the study itself fundamentally unethical?
Swedish researchers withheld the established preventive intervention for postdates pregnancy deaths to see what would happen and — not surprisingly — babies died postdates pregnancy deaths. That type of study is never ethical and no informed consent procedures can ever make exposing patients to preventable deadly risks ethical.
Their excuse?
There is no international consensus on how to manage healthy pregnancies lasting more than 40 weeks, although it is generally accepted that there is an increased risk of adverse effects for mother and baby beyond 41 weeks.
But there is complete international consensus on how to manage pregnancies beyond 42 weeks; induction is the established treatment and has been for decades.
These two charts demonstrates why.
This is a chart of stillbirth rates by gestational age.
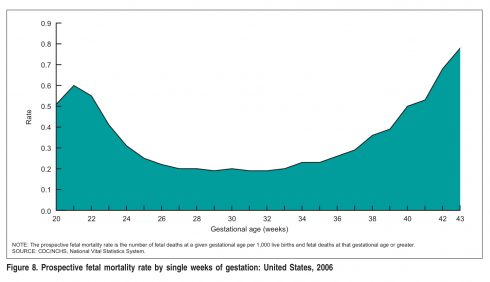
You can see that stillbirth rates begins to rise from about 36 weeks of pregnancy onward and rise steeply after 41 weeks.
Why don’t we deliver every baby at 36 weeks? Because it makes no sense to deliver a baby early to prevent stillbirth if that increases the chance that the baby will die in the days and weeks after birth.
This chart shows neonatal and infant mortality by gestational age:
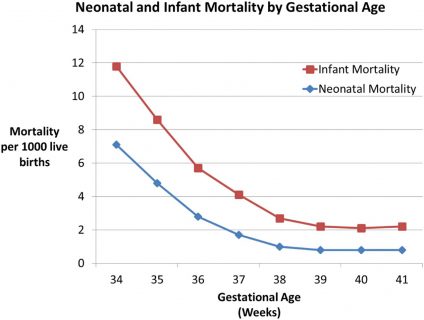
Mortality reaches the lowest rates at 39 weeks. If we want to minimize both the risk of stillbirth and the risk of neonatal death, the optimal time for delivery is 39 weeks.
There is as yet no consensus on whether routine induction should be offered at 39 weeks, 40 weeks or 41 weeks. But there is complete consensus that all women should be induced by 42 weeks. The stillbirth rate jumps precipitously from 0.5/1000 at 41 weeks to 0.75/1000 at 43 weeks. The stillbirth rate at 39 weeks, in contrast, is 0.3/1000.
…[T]he Swedish post-term induction study (Swepis) set out to survey 10,000 women at 14 hospitals.
Women in their 40th week of pregnancy were invited to join the study and divided randomly into two groups, with labour induced at the beginning of either week 42 or week 43, unless it occurred spontaneously.
Given what we know, what should researchers have expected to happen?
If 10,000 women reached 42 weeks, we would expect 5 stillbirths and if they reached 43 weeks we would expect 7-8 stillbirths.
That was an unacceptable, unethical risk. But the Swedish researchers managed to exceed the worst expectations:
When abruptly halted in October 2018, the study had involved only a quarter of the target number of expectant mothers. But the six deaths were already judged to indicate a significantly increased risk for women induced at the start of week 43. No infants died in the group whose pregnancies were ended a week earlier.
The researchers represent their findings as a new discovery:
The immediate consequences of the study “may be a change of the clinical guidelines to recommend induction of labour no later than at 41+0 gestational weeks”, its author concludes.
Sahlgrenska hospital announced on Thursday that it would change its pregnancy management policies based on the results of Swepis trial.
“We have awaited the scientific analysis showing that it is really true that there is a greater risk of waiting two weeks beyond term,” the head of childbirth operations at the hospital told Swedish television.
But there was NEVER any question that it was true. So why did the researchers, most of whom appear to be midwives, embark on this fundamentally unethical study? Because they can’t handle the truth that interventions often produce better outcomes than “unhindered” natural childbirth.
Contemporary midwifery is at a crossroads.
The foundation of contemporary midwifery is:
1. The belief that childbirth interventions inevitably lead to more interventions, often culminating in a C-section and therefore a bad ‘experience.’
2. The quest for a better childbirth experience is justified by the fact that “scientific evidence shows” that it is also a safer experience.
Hence the crossroads. One direction would confirm the claim that midwifery is about adherence to scientific evidence; the other would represent a rejection of scientific evidence in favor of doctrine. Sadly, it looks like midwives are searching desperately for any fig leaf that would cover a naked rejection of high quality science in favor of doctrine.
To cater to their own prejudices, they embarked upon a study that — predictably — killed babies. They should be held to account for letting babies die because of their irresponsible, unethical denial of established obstetrical care.